There’s no getting away from it, the digital age is here technology is evolving! The technology behind dental implants is evolving in exciting ways, making scientific use of cutting edge materials and technologies. Over the past few decades civilizations have attempted to solve the problem of tooth loss by implanting some type of “foreign material” into the jawbone. But since then, dental implants have certainly come a long way.
Advancement of Dental Implant Technology
Dental implant technology has advanced greatly leading to more cost effective procedures. Usually when a patient loses teeth due to trauma or disease, bone loss makes it difficult or impossible to use dentures or dental implants. But to every problem there’s usually a solution…bone grafting, a surgical procedure that replaces bone, is now being used to serve as support for dental implants and replacement teeth. The use of titanium mesh is often needed as a tent over the bone graft to support the graft’s shape and volume while the new bone grows. The downside is that titanium mesh can be logistically challenging and time-consuming to form and position in the patient, and it can irritate the soft tissues in the mouth.
Technique to Create Position Titanium Mesh
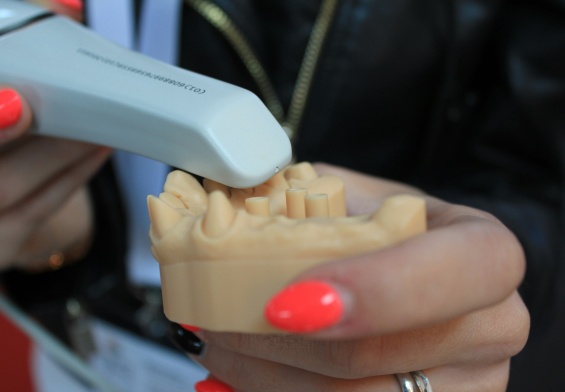
Journal of Oral Implantology shared a case letter describing a technique to create and position titanium mesh to improve guided bone regeneration. In collaboration, doctors from Loma Linda University, King Khalid University, and King Saud University encountered a patient who had several missing front teeth due to an injury that resulted in a large gap referred to as a bony defect. They decided to begin with a bone graft, followed by dental implants that would support the replacement teeth. They then created a virtual 3D model of the patient’s mouth and bony defect, then, with a computer program, they determined the correct position and placement of the bone graft based on the desire location of replacement teeth. They 3D printed a model and fabricated the titanium mesh to fit the intended bone position and volume. Lastly, they filled the titanium mesh with bone harvested from a remote location in the patient’s mouth and secured it in the site of the missing teeth with fixation screws.
How the Titanium Mesh Helps
The digital creation of the titanium mesh made it possible to ensure that the material was the precise shape and volume needed for the patient’s bone defect. This reduced the chance that the titanium mesh would cause an unfavorable outcome during healing, including mesh exposure and irritation. While in surgery they ensured the proper placement of the titanium mesh and bone graft with a positioning jig fabricated from a clear plastic mold that used the existing teeth to hold the mesh in place while it was being secured. Ultimately, to improve wound healing and bone stability, they applied fibrin membranes rich in platelets.
The Future of Dental Implants
This technique ensures precise augmentation of the bony defect and an accurate positioning of the mesh. In conclusion, prefabrication of titanium mesh also reduces surgical time and ensures that the location of replacement teeth will be correct. For the future, the goal is to improve fabrication of the positioning jig as well as to determine the dental procedures for which this technique would be appropriate.