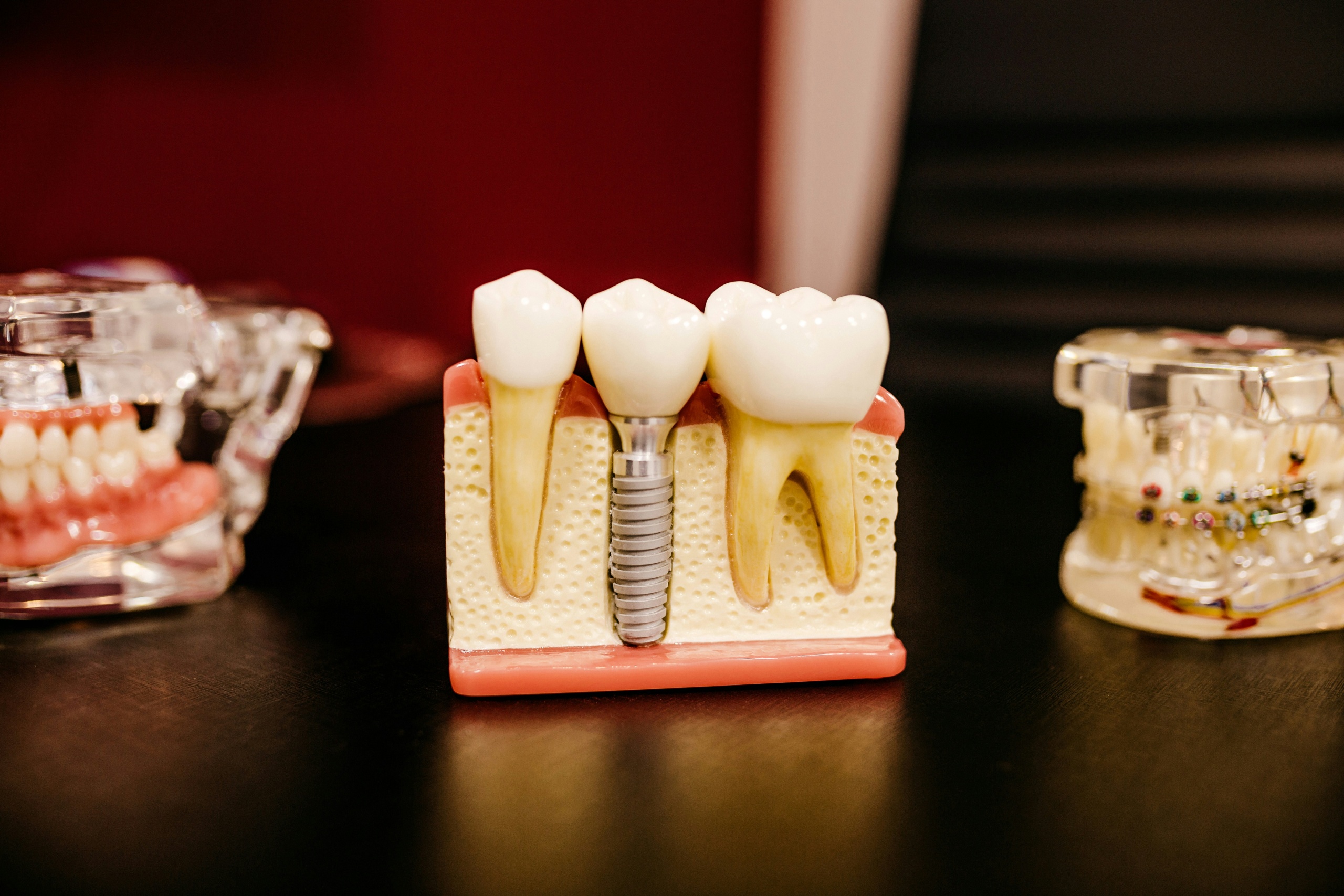
You’re on a quest for that “Hollywood Smile”, that perfect positioning of teeth, lips, and gums. Seeking such a primary driver of modern cosmetic dentistry has probably led you to research some aesthetic improvements. Many patients see these smile makeovers as just surface level, but in reality they’re anything but.
In today’s image-driven world, social trends and filtered beauty standards often influence cosmetic decisions, especially in the era of Snapchat Dysmorphia and smile expectations.
Procedures like dental veneers are popular because they mask imperfections. But they depend on the existing tooth structure, and can fracture. That’s why dental implants have become the gold standard for those seeking more permanent, robust smile rehabilitations.
For many patients considering implants, bone grafting for dental implants is the step that determines whether the procedure will succeed long term.
A permanent restoration’s success depends on the underlying foundation, the one beneath the gums. Solidifying that foundation often requires a procedure called bone grafting. Those worlds might sound intimidating, but data from massive clinical studies proves its 97.83% success rate for your new smile.
That means fewer than 3 out of every 100 implants fail, even in complex cases requiring augmentation.
Quick Answer: Do I Need Bone Grafting Before Dental Implants?
The answer depends on how much jawbone remains after tooth loss. If there’s not enough bone volume, bone grafting restores the structural foundation necessary for implant stability and osseointegration.
Large-scale research involving over 158,000 implants shows a 97.83% success rate when implants are placed with simultaneous grafting. Augmentation does not increase failure risk and often improves mechanical stability.
Common related questions:
- Is bone grafting necessary for dental implants? It’s necessary when bone loss prevents stable placement.
- How long after bone graft can I get implants? Healing usually takes 3–6 months, depending on graft size. If you’re planning your full treatment timeline, here’s a breakdown of how long dental implants take in NJ.
- How painful is bone grafting for dental implants? Most patients report mild to moderate soreness that resolves within several days.
- What are the risks of bone grafting in dental implants? While complications are uncommon, potential risks may include infection, delayed healing, graft resorption, or incomplete integration, particularly in smokers or patients with uncontrolled systemic conditions.
Here’s an infographic for quick reference:
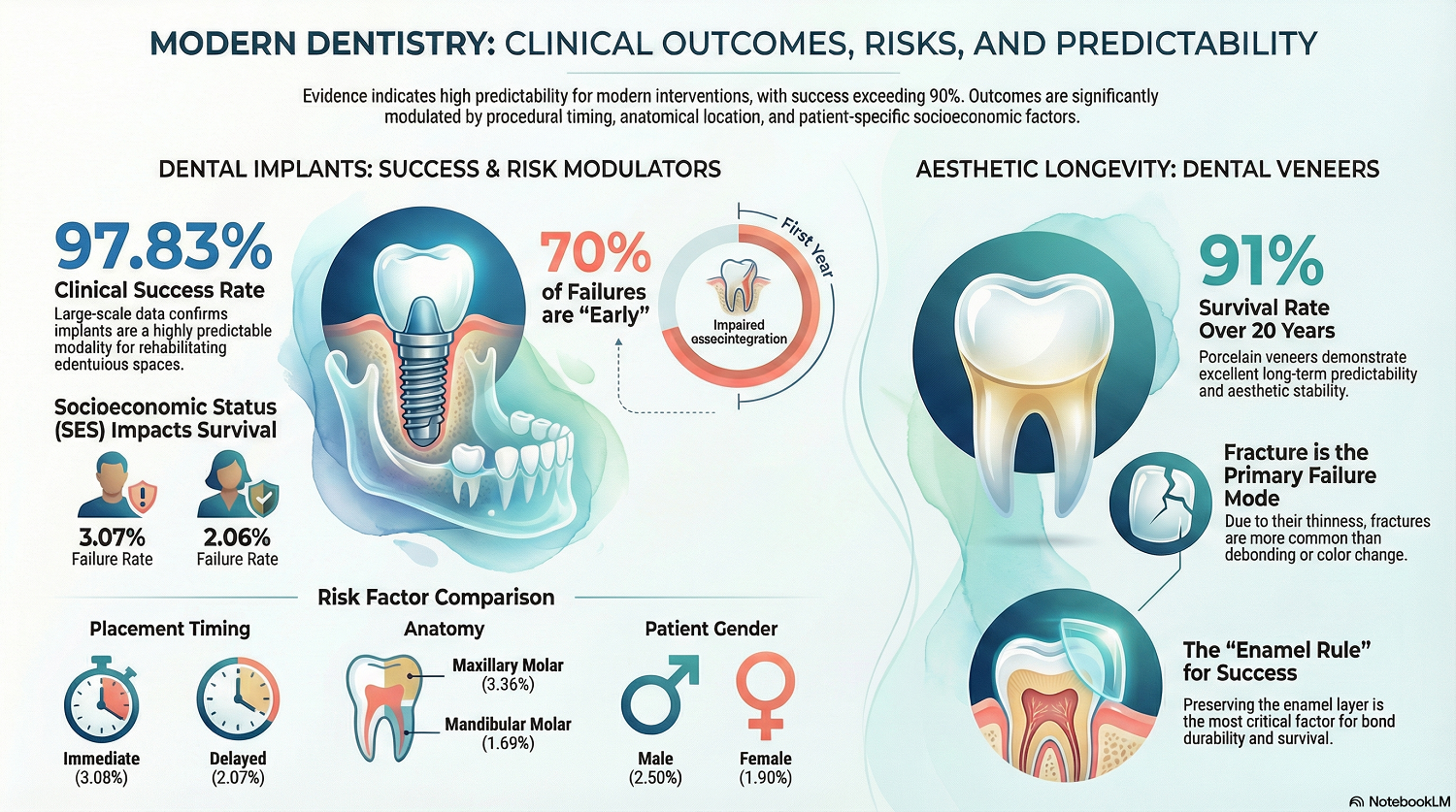
Why Jawbone Volume Is Critical for Bone Grafting for Dental Implants
A dental implant’s clinical success is directly correlated to adequate alveolar bone volume. This is the bone that anchors the implant in place right after the surgery. Without enough alveolar bone, the implant won’t be able to undergo osseointegration.
Osseointegration is the process where a titanium implant forms a direct structural and functional connection with your living bone, essentially functioning like a natural tooth root.
Unfortunately, tooth loss almost invariably leads to progressive bone loss, known as alveolar ridge resorption. This bone loss can be caused by trauma, infection, or the simple lack of mechanical stimulation that comes from a missing tooth. So, a large proportion of patients need bone augmentation to create a viable site for an implant.
This is why bone grafting for dental implants is often recommended before or during implant placement.
What Is Guided Bone Regeneration (GBR) for Dental Implants?
Dentists use a variety of restorations to fix these anatomical deficiencies, and Guided Bone Regeneration is one of the most common. GBR involves “guiding” the body into rebuilding the missing bone via specialized particulate grafts and barrier membranes. Tons of research has gone into these procedures over the last decade, and now they’re an integral part of implant procedures.
Patients sometimes worry about the risks of bone grafting in dental implants and whether adding a graft increases complication rates. A common patient concern is whether adding a bone graft makes the implant more likely to fail. That’s a concept the scientific community calls the “complexity hypothesis” rearing its ugly head.
But, large-scale research supports the “stabilization hypothesis.” That suggests that augmentation actually reduces risk by restoring the local anatomy and enhancing the site’s mechanical stability. Data from over 158,000 implants confirms that implants placed in augmented sites achieve clinical success rates statistically indistinguishable from those placed in native bone.
Bone Grafting vs. No Grafting: What’s the Difference?
If there’s not enough bone volume, an implant without grafting is more likely to experience instability.
Without grafting:
- Insufficient primary stability
- Increased early failure risk
- Compromised osseointegration
With grafting:
- Restored anatomical support
- Improved mechanical stability
- Comparable long-term success to native bone
The research is clear. Bone grafting for dental implants increases predictability, not risk.
The 97.83% Proof: Clinical Success in the Real World
The numbers don’t lie, which is why they’re important factors when deciding between cosmetic options. An analysis of 158,824 implants between 2014 and 2022 showed implants with simultaneous bone grafting had a 97.83% success rate. That’s an astronomical statistic solidifying the superiority of dental implants compared to traditional bridges or dentures.
The Comparison to Veneers
While dental veneers have a high survival rate, (approximately 91% over 20 years) they’re fundamentally different from implants. Veneers are thin ceramic layers that are bonded to the surface of the tooth. They’re highly susceptible to fracture, the primary cause of veneer failure.
If you’re comparing long-term structural solutions versus cosmetic masking, it’s helpful to understand exactly what happens to your teeth under veneers before deciding which path makes sense.
In contrast, an implant replaces the entire root system, providing functional strength and stability that a surface restoration can’t.
The Critical First Year After Bone Grafting and Implant Placement
Any new restoration is most susceptible to failure during the first year. Research shows 70% of implant failures happened in the first year. Usually, it was because the implant failed to osseointegrate properly.
That’s where the bone grafting for dental implants comes in. The whole purpose is to help patients clear that early failure window by providing the volume the bone and implant need to successfully fuse. Once this initial window is passed, late failure rates drop to approximately 0.65% annually.
Recovery Timeline: How Long After Bone Grafting Can Implants Be Placed?
Healing time depends on the size and location of the graft.
- Minor grafting: Implant placement may occur simultaneously
- Moderate grafting: 3–4 months healing
- Larger ridge augmentations: 4–6 months healing
During this period, the graft integrates and new bone forms, creating a stable site for implant placement. Most patients return to normal activities within a few days after the grafting procedure.
Personalized Risk: Why Your Habits and Health Matter
Dental implants have a stupendously high success rate, but it’s not universal. Several demographic and lifestyle factors can influence the longevity of dental implants. They may increase the risks of bone grafting in dental implants if not properly managed.
- Tobacco Use: Smoking remains a primary predictor of failure. It significantly impairs the body’s ability to heal and integrate with the implant.
- Systemic Health: Conditions like diabetes can impact gum health and worsen blood sugar control. That in turn increases the risk of complications around the implant site.
- Anatomic Location: The upper jaw (maxilla) generally has a higher failure rate than the lower jaw (mandible). Specifically, maxillary molars exhibit a 3.36% failure rate.
- Gender and Habits: Studies have found that male patients have a slightly higher failure rate (2.5%) compared to females (1.9%).
Key Takeaways: Bone Grafting for Dental Implants
- Bone grafting restores lost jawbone volume needed for implant stability
- Guided Bone Regeneration is a predictable and widely used technique
- Over 158,000 implants show a 97.83% success rate with augmentation
- Most implant failures occur within the first year
- Bone grafting recovery time for dental implants usually ranges from 3–6 months
- Smoking and systemic health conditions influence outcomes
- The risks of bone grafting in dental implants are low and manageable with proper case selection
- Bone grafting does not increase failure risk and often improves stability
Investing in Your Future Health
Modern high-tech dentistry has twisted bone grafting from a complex obstacle into a routine procedure ensuring a 97.83% success rate for implants. By restoring anatomical integrity, contemporary augmentation techniques allow patients to achieve the “Hollywood Smile” they desire without compromising long-term biological health.
True confidence doesn’t just come from having white teeth. It comes from knowing your smile is built on a foundation that will last a lifetime. Your mouth is a metric of your systemic well-being, and taking your oral health seriously is one of the most important decisions you can make for your future.
Protecting that foundation is one of the smartest ways to protect your smile investment in New Jersey.
Don’t settle for a quick fix that might fracture in a few years. If you are considering a smile makeover, ask your provider about the long-term benefits of dental implants and whether bone grafting for dental implants is necessary in your case.
Ready to build a smile that lasts a lifetime? Schedule a consultation today to see how modern implant technology can provide the permanent, successful results you’ve been looking for.
Resources
Abbasi MS, Lal A, Das G, et al. Impact of Social Media on Aesthetic Dentistry: General Practitioners’ Perspectives. Healthcare (Basel). 2022;10(10):2055. Published 2022 Oct 17. doi:10.3390/healthcare10102055
Alghazzawi TF. Clinical Survival Rate and Laboratory Failure of Dental Veneers: A Narrative Literature Review. J Funct Biomater. 2024;15(5):131. Published 2024 May 16. doi:10.3390/jfb15050131
Borges CM, Krishnamurthy M. Are We Getting Any Better? A Critical Analysis of Selected Healthy People 2020 Oral Health Indicators in 1999-2004 and 2013-2016, USA. Int J Environ Res Public Health. 2022;19(9):5250. Published 2022 Apr 26. doi:10.3390/ijerph19095250
Centers for Disease Control and Prevention – About Oral Health
Findler M, Doron H, Mann J, Chackartchi T, Tobias G. Clinical Success Rates of Dental Implants with Bone Grafting in a Large-Scale National Dataset. J Funct Biomater. 2026;17(1):46. Published 2026 Jan 15. doi:10.3390/jfb17010046
Yashpal S, Raghunath A, Gencerliler N, Burns LE. Exploring Public Perceptions of Dental Care Affordability in the United States: Mixed Method Analysis via Twitter. JMIR Form Res. 2022;6(7):e36315. Published 2022 Jul 1. doi:10.2196/36315