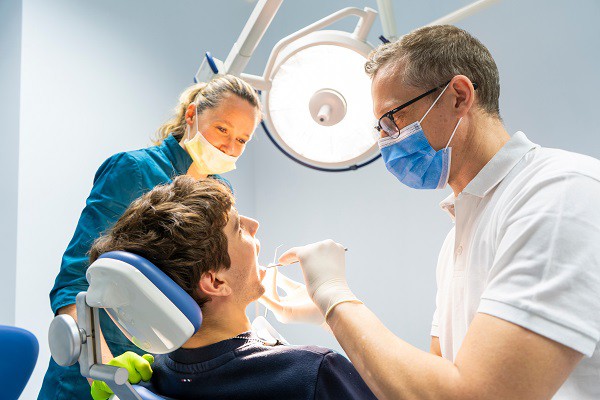
Tooth pain derails the day in a heartbeat. Dull aches can be easily ignored, but consistent pain that lingers after morning coffee, flares up when biting, or otherwise keeps coming back is harder to dismiss. That’s usually what leads people to ask themselves, “Do I need a root canal?”
The short answer is that it depends. Tooth pain has numerous potential causes, including gum irritation, worn enamel, a small cavity, grinding, or sinus pressure. But if the pain feels like it’s coming from deep inside one specific tooth, that’s cause for concern.
Root canal treatment is common, and it is usually meant to save a tooth, not remove it. The American Association of Endodontists reports that more than 15 million teeth are treated and saved each year with root canal, or endodontic, treatment.
When decay, trauma, or a crack reaches the pulp, root canal therapy may allow the dentist to remove infected tissue while keeping the natural tooth in place. Knowing what a root canal actually treats alleviates that fear for many patients. “Killing” the tooth isn’t the objective; quite the contrary. It’s about saving a tooth by cleaning the inside of it.
Do I Need a Root Canal? Signs That Deserve a Dental Exam
A root canal may be needed when the soft pulp inside the tooth becomes inflamed, infected, or dead. The pulp sits beneath the enamel and dentin. It contains nerves, blood vessels, and connective tissue.
Some warning signs are obvious, like swelling near one tooth. Others are easier to explain away at first, especially when the pain comes and goes.
Common warning signs include:
- Severe pain while chewing or biting
- A pimple-like bump on the gum
- A chipped or cracked tooth
- Lingering sensitivity to hot or cold
- Swollen or tender gums
- Deep decay or darkening around the tooth
None of these symptoms by themselves guarantee a root canal. They tell the dentist which teeth to evaluate for one.
Lingering Hot or Cold Sensitivity
That quick zing from sipping ice water isn’t always a root canal sign. Many things can cause that kind of sensitivity, like exposed roots, worn enamel, whitening products, or regular cavities. If the zing becomes more than quick, that’s a different story. When a tooth keeps aching after removing the cold stimulus, that’s a sign of nerve irritation that warrants further testing.
Pain that seems to move across several teeth can be confusing, which is why it can help to compare one-tooth pain with why all your teeth hurt suddenly. A single inflamed tooth can feel surprisingly broad at first, especially when the jaw is tense and the person keeps checking the area with their tongue.
The same goes for heat sensitivity. Some patients notice it during an ordinary moment, like taking a sip of coffee in the morning and feeling one tooth continue to throb after the cup is back on the counter.
Pain When Biting or Chewing
Biting pain often gives the dentist useful information. It may point to deep decay, a cracked tooth, a loose filling, or inflammation near the root. Pain on release can be especially suspicious for a crack. The tooth may feel fine until pressure comes off, then a sharp pain hits for a second.
Some painful teeth need more than a basic visual exam, especially when the canal anatomy is difficult or an older root canal hasn’t healed properly. Some cases might involve an in-house endodontist to trace the source of pain more precisely.
When Tooth Pain Becomes More Urgent
Some toothaches can wait for a scheduled dental visit. Swelling, fever, drainage, or trouble swallowing can’t.
A tooth abscess can cause severe throbbing pain, fever, swelling in the face or neck, tender lymph nodes, foul odor, or bad-tasting fluid if it drains. Pain with chewing or biting can also appear when there’s an infection.
If swelling, severe pressure, or spreading pain makes normal eating difficult, a same-day dentist appointment may be the safer choice. Waiting for a routine cleaning slot can give an infection more time to fester beyond the tooth.
Face or neck swelling with fever should be treated with extra care. Trouble breathing or swallowing calls for emergency care.
Swelling, Fever, or Trouble Swallowing
A small swollen spot near one tooth can be the first visible sign of infection. A gum boil, pus, or a bad taste in the mouth can also point toward an abscess. These abscesses don’t just go away on their own. They can rupture, and the pressure will drop and the tooth might feel better. But there’s still an underlying infection that needs attention.
It’s easy to miss that detail, because pain relief can mislead people into thinking they’ve healed despite the infection’s lingering presence. A common sign of leftover infection is fever. It’s a signal the body’s reaction to the infection proliferating. Facial swelling, neck swelling, or difficulty swallowing should not be watched casually at home.
Why a Dentist May Recommend Root Canal Treatment
Root canal treatment cleans infected or inflamed tissue from inside the tooth. During treatment, the dentist removes infected pulp, cleans the inside of the tooth, fills the space, and seals the tooth.
Pulp can become infected after a deep cavity, repeated dental work, a cracked or fractured tooth, or an injury. Even if there aren’t any visible cracks or chips, those teeth might still need care.
A treated tooth often needs protection afterward. Because back teeth take heavy chewing force, a dental crown is often used after root canal treatment to restore strength and protect the remaining tooth structure.
A root canal is not the only possible answer. A painful tooth may need a filling, crown, gum care, bite adjustment, night guard, or another treatment once the dentist finds the cause.
Deep Decay, Cracks, Old Fillings, and Dental Trauma
Cavities, specifically, can stay under the radar until they get to the pulp. By the time they start to hurt, there’s already a deeper problem than what shows up in the mirror. Cracks can also be hard to spot in the mirror. Even if the tooth looks fine on the surface, it can still hurt when biting on a specific area.
Old fillings and crowns can create another problem. Decay can form around an edge, under a restoration, or in a spot that does not look dramatic from the outside. Dental injuries can also take time to show themselves. A tooth that was hit may not darken or become painful until months later.
The exam is easier when the dentist knows the full story. Pain triggers, old dental work, swelling, and recent injuries are all part of what patients should tell their dentist before they can recommend treatment.
How Dentists Decide If a Root Canal Is Needed
Dentists don’t decide whether someone needs a root canal off pain alone. They look for what’s causing that pain and test whether the pulp responds normally.
Before recommending treatment, a dentist may use X-rays, tap on the tooth, apply hot or cold, or use electric pulp testing. These checks help show whether the pulp is still alive, irritated, infected, or no longer responding.
That exam usually uncovers much more than the pain description itself. What feels like several teeth may only be one tooth. What feels like upper tooth pain may actually be sinus pressure. Gum infection can sit close enough to a tooth root that the person feels sure the tooth is the problem. X-rays can be helpful here; they let the dentist see below the surface. They might spot decay near the pulp, bone changes near the root tip, an abscess, or problems around old dental work.
Why Testing Changes the Answer
Temperature testing gives the dentist a clue about the nerve. A tooth that reacts sharply and keeps aching after cold may behave differently from a tooth that does not respond at all.
Bite testing can show where pressure causes pain. Tapping can show whether the tissue around the root is inflamed.
Gum measurements may also be needed. Sometimes the pain is not coming from the pulp, even when it feels like it is.
That is why a root canal question needs more than a pain description. The dentist has to match the symptoms to the tooth, the X-ray, and the test results.
Do I Need a Root Canal If the Pain Goes Away?
Pain that fades can feel reassuring. The tooth could have calmed down. Or the nerve inside it could be dying. Or an abscess just ruptured and is now draining. That’s a common cause of misleading pain. An abscess rupturing can bring much-needed relief, but still requires dental treatment.
Fear can also change the timeline. People who have had a difficult dental visit in the past may wait until the pain is harder to manage, and sedation dentistry can make treatment feel more manageable while the dentist addresses the source of the problem.
Common Questions Patients Ask Before Calling
What symptoms mean I might need a root canal?
Lingering hot or cold sensitivity, pain when biting, swollen gums, a gum boil, tooth darkening, or severe throbbing pain may mean a root canal is possible. The pattern matters too. Pain that keeps returning in the same tooth deserves more attention than a quick sensitivity twinge that fades right away.
Does tooth pain always mean I need a root canal?
No. Tooth pain can come from cavities, gum disease, grinding, sinus pressure, cracks, or sensitivity. The dentist has to find the source before recommending treatment.
How long should tooth pain last before I call a dentist?
Tooth pain that lasts more than a day or two, keeps returning, interrupts sleep, or makes chewing difficult should be checked. Pain with swelling, fever, drainage, or trouble swallowing calls for faster care.
Can antibiotics fix a tooth infection?
Antibiotics may help when an infection has spread, but they do not remove infected pulp from inside a tooth. The source often needs dental treatment.
Is a root canal painful?
Root canal treatment is designed to relieve tooth pain. Dentists use local anesthesia during treatment, and once treatment is complete, the pain felt before the procedure should no longer be present.
What to Do With Tooth Pain That Keeps Coming Back
When someone asks, “do I need a root canal?” the pain has usually crossed a line from annoying to concerning. Lingering sensitivity, bite pain, swelling, fever, recurring pain, or tooth darkening all deserve a closer look.
The most useful thing a patient can bring to the appointment is a clear description of what happens. Which tooth hurts, what triggers it, how long it lasts, whether it wakes them up, and whether swelling has appeared.
A dental exam can separate a treatable cavity from an infected pulp, a cracked tooth, or an abscess. That answer is much better to get early, before the pain becomes harder to ignore.